Regenerative medicine continues to reshape modern healthcare by focusing on repairing, replacing, or regenerating damaged tissues and organs. At the core of this innovation are specialized cell types that drive healing and functional recovery. Understanding these cells helps clinicians and patients appreciate how regenerative therapies deliver measurable outcomes across multiple medical fields.
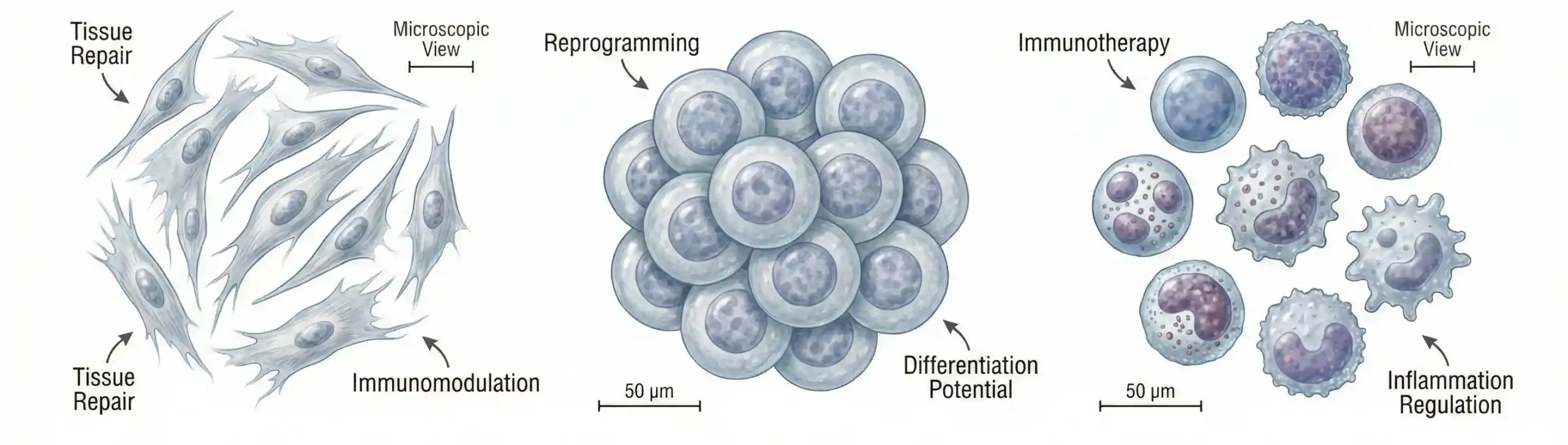
Regenerative medicine therapies rely on the biological potential of living cells. These cells promote repair by reducing inflammation, stimulating tissue growth, and restoring normal cellular function. As research advances, the clinical applications of regenerative medicine continue to expand across orthopedics, neurology, cardiology, and aesthetic medicine.
Mesenchymal regenerative cells remain among the most widely used cell types in regenerative medicine therapies. They are commonly sourced from bone marrow, adipose tissue, and umbilical cord tissue.
Mesenchymal Regenerative Cells support healing by:
Modulating inflammation
Enhancing tissue regeneration
Supporting immune system balance
Because they adapt to different tissue environments, MSCs are frequently applied in joint, spine, and soft tissue treatments.
Hematopoietic regenerative cells primarily contribute to blood and immune system regeneration. These cells have long been used in bone marrow transplantation.
In regenerative medicine, Hematopoietic Regenerative Cells are vital for:
Immune system restoration
Blood cell regeneration
Supportive therapy after intensive treatments
Their established clinical history makes them one of the most trusted regenerative cell types.
Induced pluripotent regenerative cells are adult cells reprogrammed to behave like embryonic stem cells. This innovation allows researchers to create patient-specific cells without ethical concerns.
Induced Pluripotent Regenerative Cells show promise in:
Personalized regenerative medicine therapies
Disease modeling
Advanced tissue engineering
Although still largely in research phases, their future clinical impact is significant.
Macrophages play a critical role in tissue repair. In regenerative medicine therapies, they help regulate inflammation and guide healing responses.
Properly activated macrophages:
Remove damaged tissue
Promote regeneration rather than scarring
Support vascular repair
This balance is essential for successful regenerative outcomes.
Regulatory T cells help maintain immune tolerance. In regenerative medicine, they reduce excessive immune responses that may interfere with healing.
Tregs contribute by:
Preventing chronic inflammation
Supporting tissue integration
Enhancing long-term treatment success
Their role continues to grow as immune-based regenerative strategies evolve.
Choosing the appropriate cell type directly influences treatment outcomes. Each regenerative medicine application requires a targeted cellular approach. Therefore, practitioner training remains essential for safe and effective therapy delivery.
To learn more about professional education in this field, explore advanced programs at IARM Training Services: https://iarm-usa.com/
National Institutes of Health – Regenerative Medicine Overview
https://www.nih.gov
Mayo Clinic – Stem Cell Therapy Explained
https://www.mayoclinic.org
International Society for Stem Cell Research (ISSCR)
https://www.isscr.org
These resources provide scientific validation and ongoing research updates related to regenerative medicine therapies.
